Retroperitoneal desmoid MRI
Retroperitoneal desmoid tumors are a rare type of benign (non-cancerous) fibrous growth that occurs in the retroperitoneum. The retroperitoneum is the part of the abdomen that lies behind the peritoneum, the lining of the abdominal cavity, and contains the kidneys, pancreas, and other structures. Understanding retroperitoneal desmoid tumors involves looking at their characteristics, causes, symptoms, and treatment options.
Characteristics
- Benign but Aggressive: While they are benign and do not metastasize (spread to other parts of the body), desmoid tumors can be locally aggressive, growing into and compressing nearby organs or structures.
- Fibroblastic Origin: They arise from fibroblasts, which are cells that form connective tissue.
- Variable Growth Rate: These tumors can vary in their growth rate; some may grow quickly, while others remain stable or even regress spontaneously.
Symptoms
Symptoms of retroperitoneal desmoid tumors are often related to their size and location:
- Asymptomatic: Many are asymptomatic, especially when small.
- Abdominal Pain or Discomfort: As they grow, they can cause pain or discomfort.
- Organ Compression: They may compress nearby organs, leading to symptoms like nausea, vomiting, changes in bowel habits, or urinary symptoms.
- Mass Effect: A palpable abdominal mass might be felt in some cases.
Treatment
Treatment options vary based on the size, location, and behavior of the tumor, as well as the patient’s overall health:
- Observation: Small, asymptomatic tumors may just be monitored with regular imaging.
- Surgery: The mainstay of treatment for symptomatic or growing tumors is surgical removal. Complete resection can be challenging due to their location and the involvement of surrounding structures.
- Radiation Therapy: This may be used as an adjunct to surgery, particularly if complete removal is not possible.
- Chemotherapy: It’s typically reserved for unresectable, rapidly growing, or recurrent tumors.
MRI appearance of Retroperitoneal desmoid
- T1-Weighted MRI: On T1-weighted images, retroperitoneal desmoid tumors generally appear as masses with a signal intensity that is similar to or slightly higher than that of muscle. They are often well-defined but can infiltrate surrounding structures.
- T2-Weighted MRI: In T2-weighted images, these tumors typically show a high signal intensity, which is a characteristic feature. This high signal intensity is due to the high water content of the myxoid matrix within the tumor. However, the signal can vary if the tumor has areas of fibrosis or low cellularity, which appear as lower signal intensities.
- STIR (Short Tau Inversion Recovery) Images: In STIR images, desmoid tumors often show a high signal intensity, helping to differentiate them from surrounding structures. This sequence is particularly useful for identifying edema or inflammation around the tumor and for delineating the extent of the tumor, especially in complex areas like the retroperitoneum.
T2 TSE coronal image shows retroperitoneal desmoid
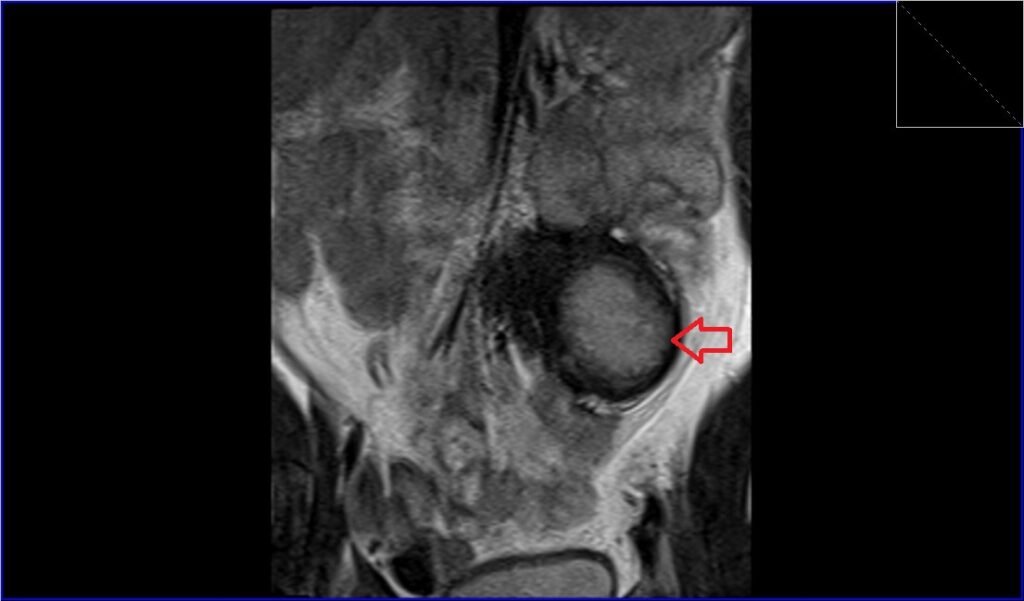
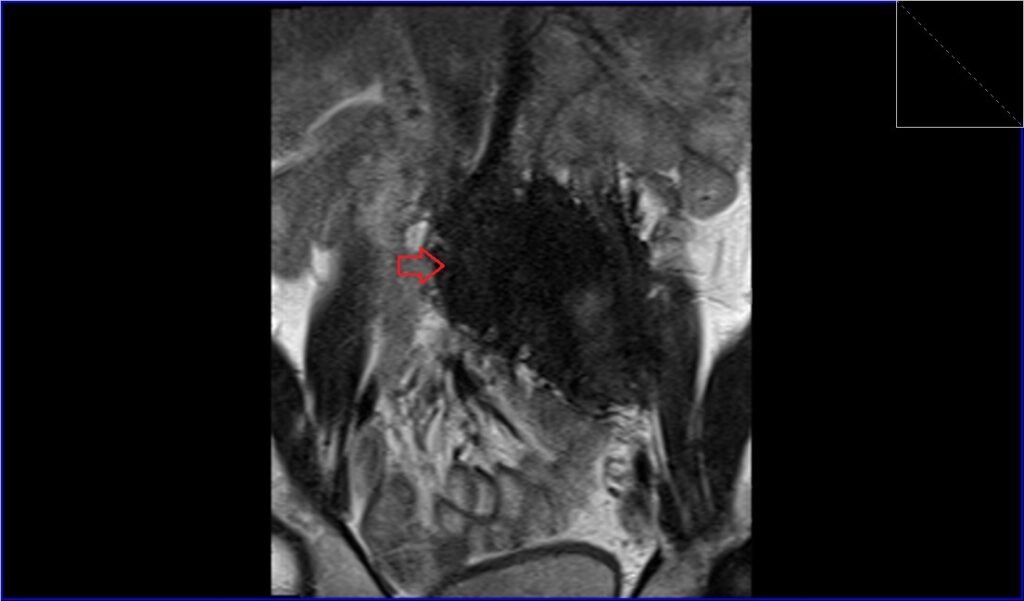
T2 TSE coronal image shows retroperitoneal desmoid
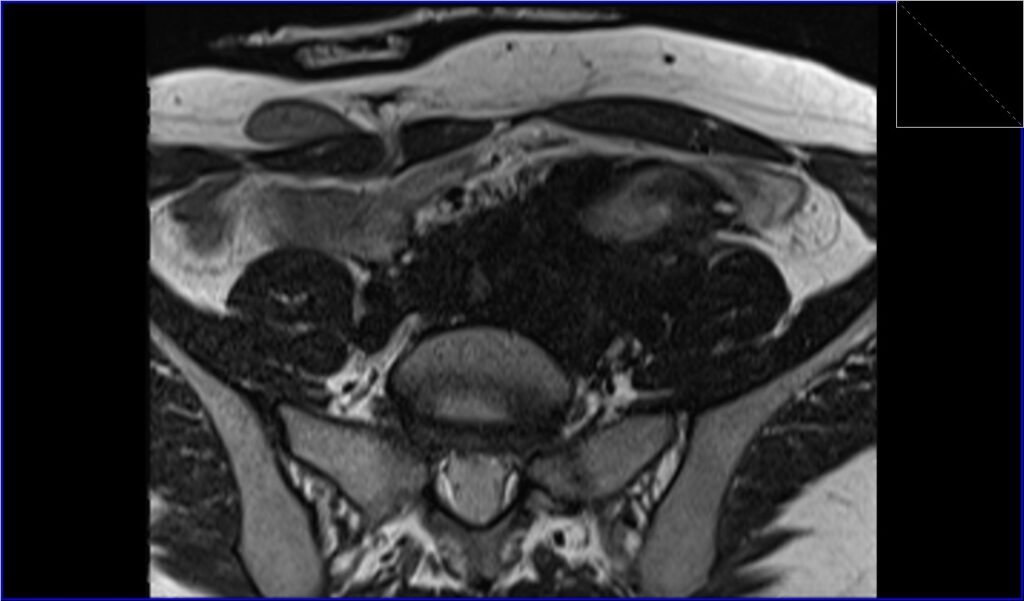
T2 TSE axial image shows retroperitoneal desmoid
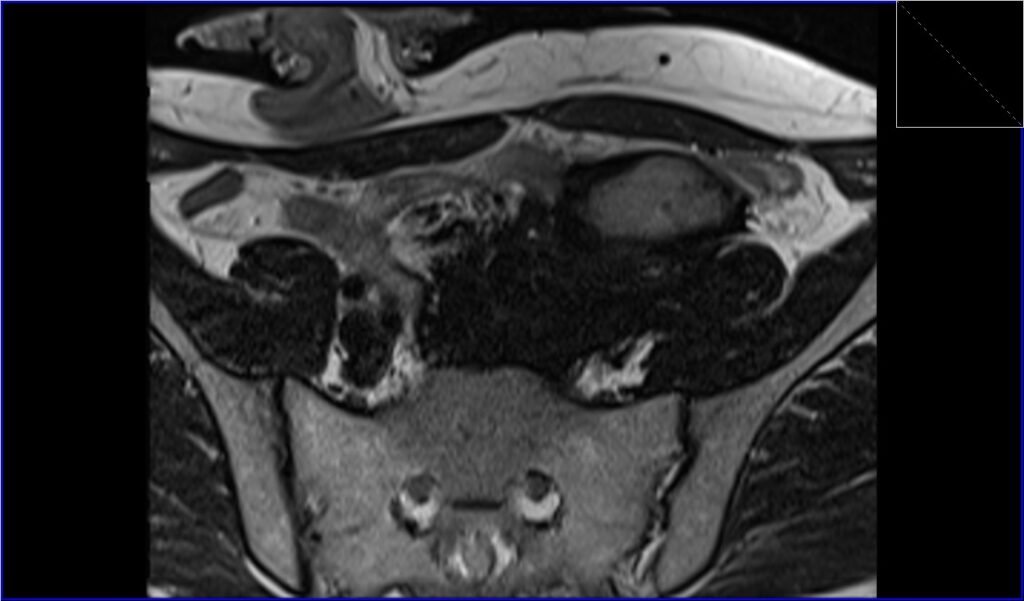
T2 TSE axial image shows retroperitoneal desmoid
References
- Mousa AH, Nukaly HY, Ahmed RA, Zubair TM, Merdad MJ, Rahman M, Shmailah EA, Bondogji R, Alshanberi AM, Khaled I. An accidental finding of a retroperitoneal desmoid tumor: case report and review of the literature. Ann Med Surg (Lond). 2023 Feb; 85(2): 246–251. doi: 10.1097/MS9.0000000000000205. PMID: 36845812. PMCID: PMC9949819.
- Lee, K.C., Lee, J., Kim, B.H., Kim, K.A., & Park, C.M. (2018). Desmoid-type fibromatosis mimicking cystic retroperitoneal mass: case report and literature review. BMC Medical Imaging, 18(29).
- Ono, H., Hori, K., Tashima, L., Tsuruta, T., Nakatsuka, S.-i., & Ito, K. (2018). A case of retroperitoneal desmoid-type fibromatosis that involved the unilateral ureter after gynaecologic surgery. International Journal of Surgery Case Reports, 47, 30-33.
- Shinagare AB, Ramaiya NH, Jagannathan JP, Krajewski KM, Giardino AA, Butrynski JE, Raut CP. “A to Z of Desmoid Tumors.” AJR. 2011; 197:W1008–W1014. DOI: 10.2214/AJR.11.7630.
