MRI Lymphoma of the Neck
Lymphoma is a type of cancer that begins in the lymphocytes, which are the disease-fighting cells of the immune system that are found in the lymph nodes, spleen, thymus, bone marrow, and other parts of the body. When lymphoma affects the lymph nodes in the neck, it is referred to as neck lymphoma, which can either be Hodgkin lymphoma (HL) or non-Hodgkin lymphoma (NHL). Both types of lymphomas can occur in the neck lymph nodes and other parts of the body.
Symptoms:
Symptoms of lymphoma in the neck can include:
- Swollen, Painless Lymph Nodes in the Neck: Often the first sign of lymphoma is painless swelling in one or more lymph node.
- Fatigue: Persistent tiredness that does not improve with rest can be a symptom.
- Difficulty Swallowing or Breathing: If enlarged lymph nodes press against the throat or windpipe.
- Coughing or Hoarseness: As a result of pressure on the throat or lungs.
- Other Symptoms: Unexplained fever, night sweats, and weight loss, Itching, loss of appetite, or a feeling of fullness due to an enlarged spleen or liver.
Treatment:
Treatment for neck lymphoma, as with other lymphomas, depends on the type (Hodgkin or non-Hodgkin), stage of the disease, the patient’s age, and overall health status. Treatment options include:
- Chemotherapy: The use of anti-cancer drugs to destroy cancer cells.
- Radiation Therapy: The use of high-energy radiation to kill cancer cells or keep them from growing.
- Immunotherapy: Treatments that use the body’s own immune system to attack cancer cells.
- Targeted Therapy: Drugs that target specific vulnerabilities in cancer cells.
- Stem Cell Transplant: The replacement of diseased bone marrow with healthy stem cells.
- Surgery: In some cases, an operation may be performed to remove an affected lymph node or other involved tissue.
MRI Appearance of Lymphoma
T1-Weighted Images (T1): On T1-weighted MRI sequences, lymphoma typically appears as a mass with intermediate to low signal intensity, which means it’s generally darker than the surrounding fat and lighter than the muscles.
T2-Weighted Images (T2): lymphoma usually have a higher signal intensity on T2-weighted images, making them appear brighter than the surrounding musculature. They are more conspicuous in this sequence compared to T1, especially when the nodes are large and confluent.
Short Tau Inversion Recovery (STIR) Images: STIR is an MRI sequence that is particularly sensitive to fluids and edema within tissues. Lymphomatous tissue will typically appear very bright on STIR images due to its high water content. The STIR sequence is also valuable in suppressing fat signal, making lymph nodes stand out more distinctly against the fatty background, which is common in areas like the neck.
Diffusion-Weighted Imaging (DWI): DWI assesses the diffusion of water molecules within tissue. Lymphomatous tissue often restricts water diffusion due to high cellularity and increased nucleic content. On DWI, lymphoma can appear as areas of high signal intensity, and on the corresponding Apparent Diffusion Coefficient (ADC) maps, they will show low signal intensity, indicating restricted diffusion. This can help differentiate lymphoma from other neck masses.
Post-Contrast T1 Images: After the administration of a gadolinium-based contrast agent, lymphomatous nodes will typically enhance on post-contrast images. However, the enhancement pattern may be variable. Homogeneous enhancement can be seen, but sometimes there is heterogeneous enhancement, particularly in large or necrotic nodes. Post-contrast sequences are particularly useful in defining the extent of the disease and in evaluating the response to treatment.
STIR coronal image shows Lymphoma
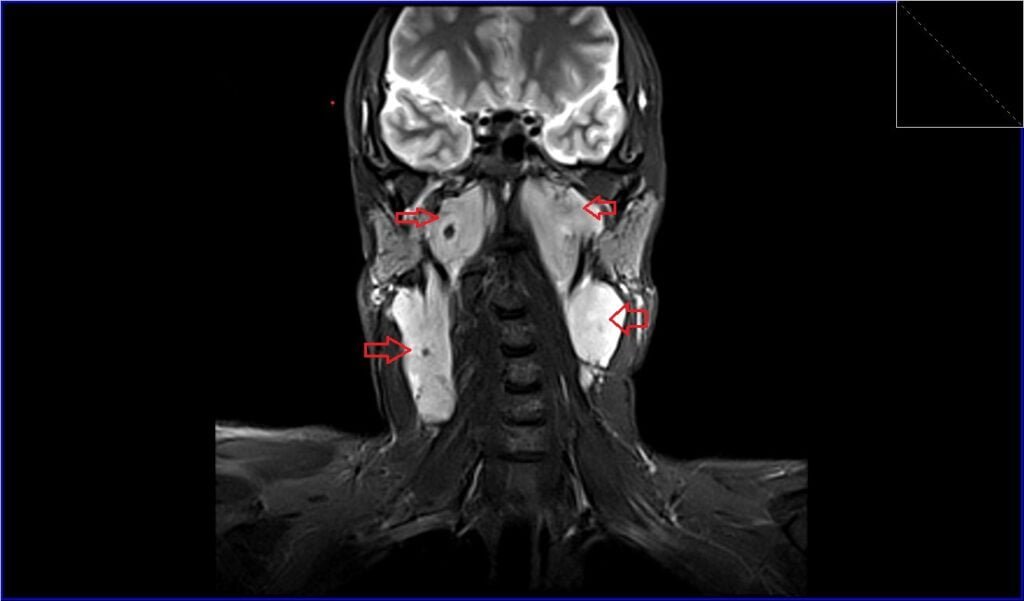
T1 coronal image shows Lymphoma

STIR axial image shows Lymphoma

T1 axial image shows Lymphoma
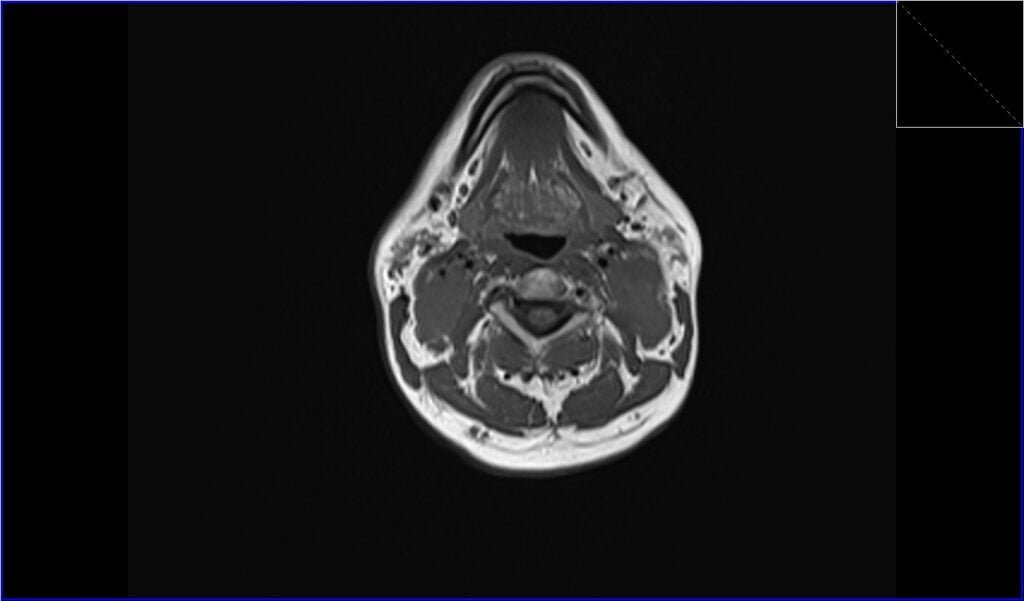
DWI axial b0 image shows Lymphoma
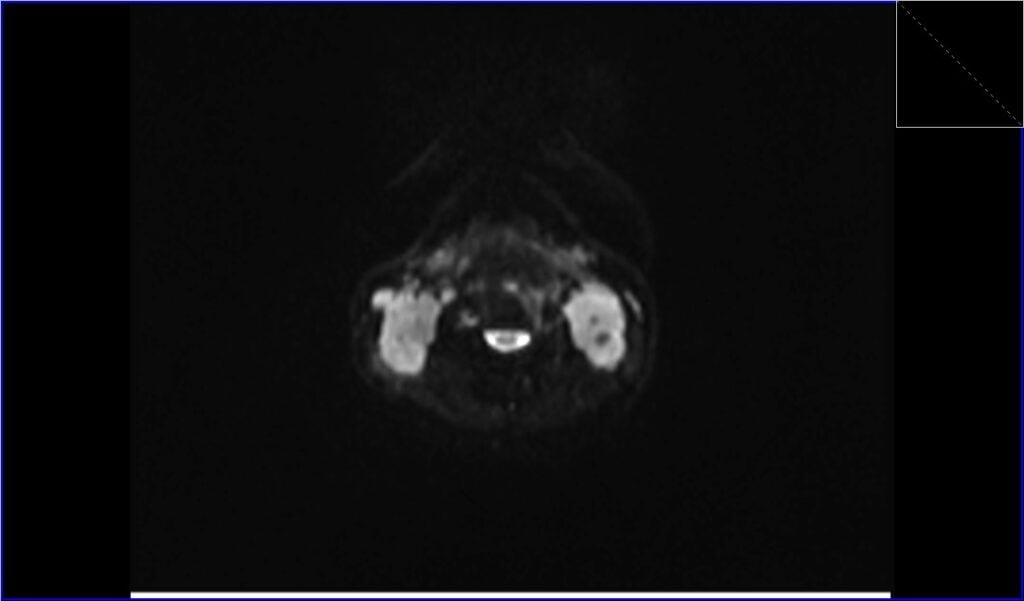
DWI axial b800 image shows Lymphoma
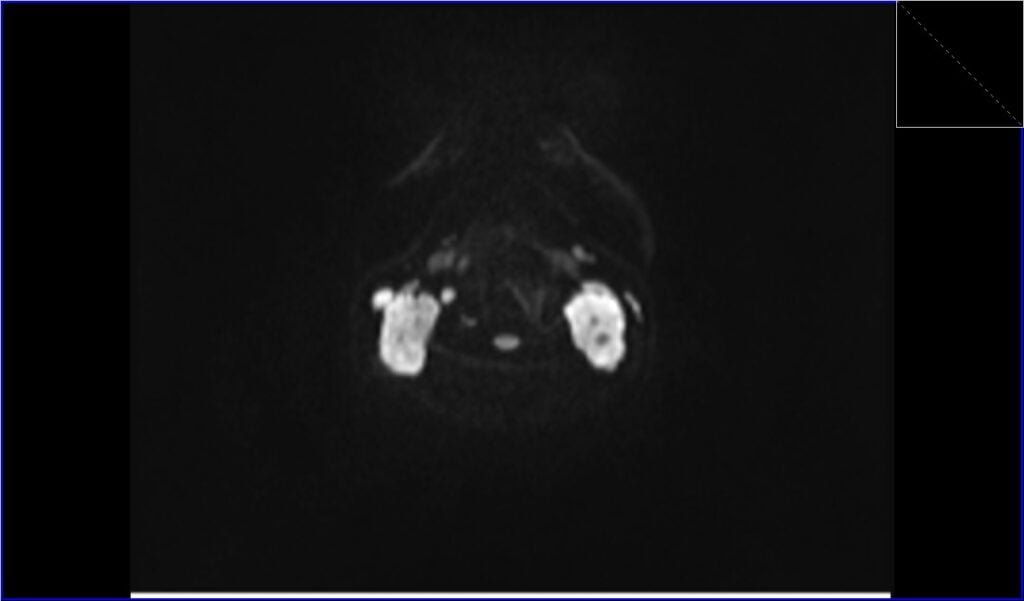
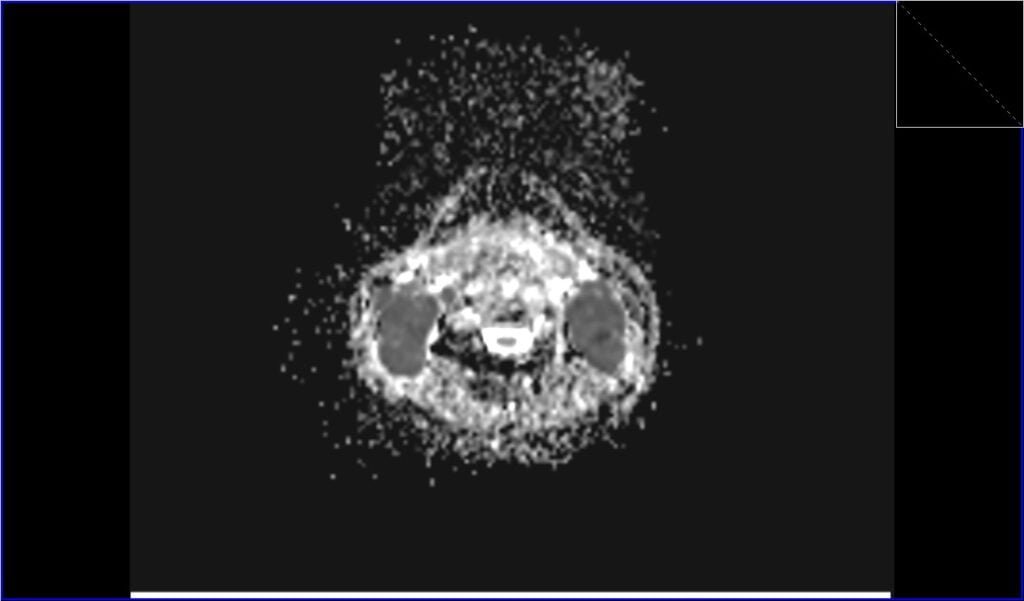
ADC axial image shows Lymphoma
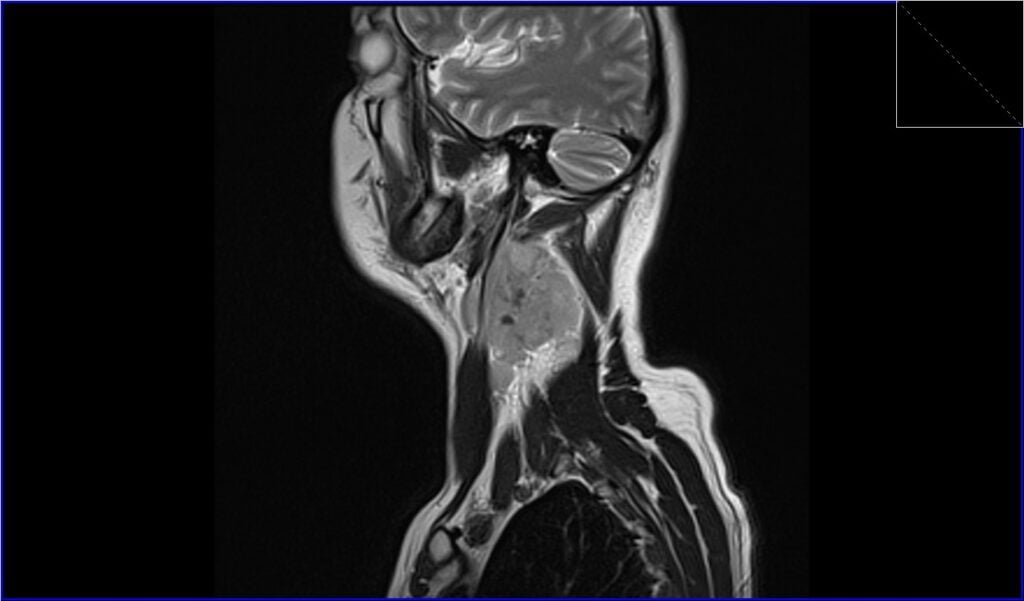
T2 sagittal image shows WLymphoma
T1 fat sat post contrast axial image shows Lymphoma

T1 fat sat post contrast coronal image shows Lymphoma

References
- King AD, Lei KI, Ahuja AT. MRI of neck nodes in non-Hodgkin’s lymphoma of the head and neck. Br J Radiol. 2004 Feb;77(914):111-5. doi: 10.1259/bjr/53555208. PMID: 15010382.
- King, A. D., Law, B. K. H., Tang, W. K., Mo, F. K. F., Raghupathy, R., Bhatia, K. S., & Lei, K. I. K. (2017). MRI of diffuse large B-cell non-Hodgkin’s lymphoma of the head and neck: comparison of Waldeyer’s ring and sinonasal lymphoma. European Archives of Oto-Rhino-Laryngology, 274(2), 1079-1087. doi: 10.1007/s00405-016-4337-2.
- DePeña, C. A., Van Tassel, P., & Lee, Y. Y. (1990). Lymphoma of the head and neck. Review Radiol Clin North Am, 28(4), 723-743. PMID: 2190267.
- Weber, A. L., Rahemtullah, A., & Ferry, J. A. (2003). Hodgkin and non-Hodgkin lymphoma of the head and neck: clinical, pathologic, and imaging evaluation. Neuroimaging Clin N Am, 13(3), 371-392. doi:10.1016/s1052-5149(03)00039-x.
- Storck K, Brandstetter M, Keller U, Knopf A. Clinical presentation and characteristics of lymphoma in the head and neck region. Head Face Med. 2019 Jan 3;15(1):1. doi: 10.1186/s13005-018-0186-0. PMID: 30606206. PMCID: PMC6317257.
- Chi, H.-S., Lee, K.-W., Chiang, F.-Y., Tai, C.-F., Wang, L.-F., Yang, S.-F., Lin, S.-F., & Kuo, W.-R. (2012). Head and neck extranodal lymphoma in a single institute: a 17-year retrospective analysis. Kaohsiung Journal of Medical Sciences, 28(8), 435-441. doi:10.1016/j.kjms.2012.02.014. PMID: 22892165.
