MRI Bilateral hip fractures
Hip fractures are serious injuries that occur in the upper part of the femur (thigh bone), near where it joins the pelvis at the hip joint. They are particularly common in older adults, largely due to weakened bones from osteoporosis and an increased risk of falling. Hip fractures can significantly affect mobility and independence, and they require prompt medical attention.
Causes
- Osteoporosis: This is the most common cause, especially in older adults. Osteoporosis weakens bones, making them more susceptible to fractures even with minor falls or stresses.
- Falls: Especially in the elderly, even a simple fall can lead to a hip fracture due to weakened bones.
- Trauma: Car accidents or other high-impact events can cause hip fractures in younger individuals with stronger bones.
- Repetitive Stress: Rarely, hip fractures can occur from repetitive motion or stress, often seen in athletes.
- Medical Conditions: Some conditions like cancer or bone diseases can weaken the bone, making it more prone to fractures.
Symptoms
- Severe Pain: In the hip or groin area following a fall or trauma.
- Inability to Move or Bear Weight: Immediately after the injury, the person might be unable to move the leg or stand.
- Stiffness, Bruising, and Swelling: Around the hip area.
- Shortened or Externally Rotated Leg: The injured leg may appear shorter and turned outward compared to the other leg.
Treatment
Initial Management
- Emergency Care: Immediate medical attention is required. This includes pain management and immobilization of the fracture.
- Assessment: X-rays, and possibly an MRI or CT scan, to assess the fracture type and plan treatment.
Surgical Treatment
Most hip fractures require surgery, which varies depending on the type and location of the fracture:
- Internal Fixation: Involves using metal screws, rods, or plates to hold the bone fragments in place while they heal.
- Hip Replacement Surgery: In cases where the fracture is severe or the hip joint is affected, a partial or total hip replacement might be necessary.
- Hemiarthroplasty: Replacing the femoral head (the ball of the hip joint) but not the socket.
Non-Surgical Treatment
- Limited to Certain Cases: Non-surgical treatment is rare, typically reserved for patients who have severe health conditions that make surgery too risky.
- Traction or Immobilization: To allow healing, though this approach is less common due to increased risks of complications.
MRI appearance of hip fractures
T1-Weighted Images: In T1 sequences, normal bone marrow is high signal (bright) because of its fat content. A hip fracture would appear as a low signal (dark) line interrupting this bright signal. This low signal represents the bone marrow edema or hematoma caused by the fracture. The fracture line itself may be subtle and difficult to detect, especially in the early stages.
T2-Weighted Images: In T2 sequences, the fluid in bone marrow edema or hematoma associated with a fracture becomes high signal (bright). Thus, a hip fracture is more conspicuous on T2 images than on T1 due to the high signal of the surrounding edema. It appears as a bright line or area within the normally lower signal intensity of bone.
STIR (Short Tau Inversion Recovery) Images: STIR is particularly sensitive to fluid and is used to suppress the fat signal, making edema or fluid appear bright. In the case of a hip fracture, the STIR sequence will show a high signal intensity (bright) area due to edema, making the fracture more detectable compared to T1 images. This sequence is beneficial for detecting subtle bone marrow edema
STIR coronal image shows Bilateral hip fractures
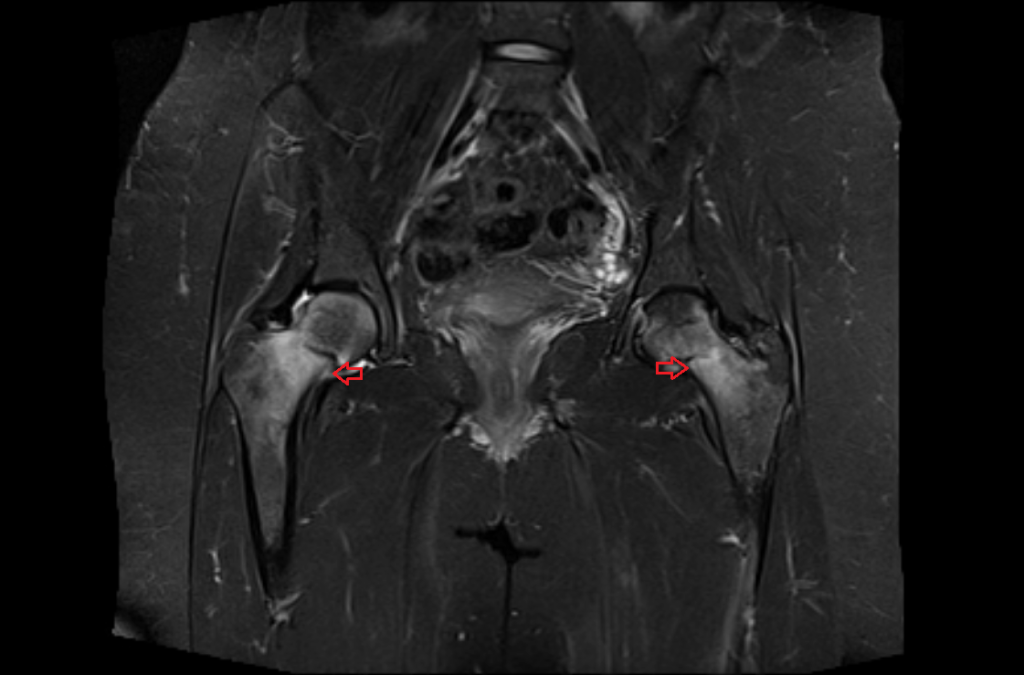
T1 coronal image shows Bilateral hip fractures

STIR axial image shows Bilateral hip fractures
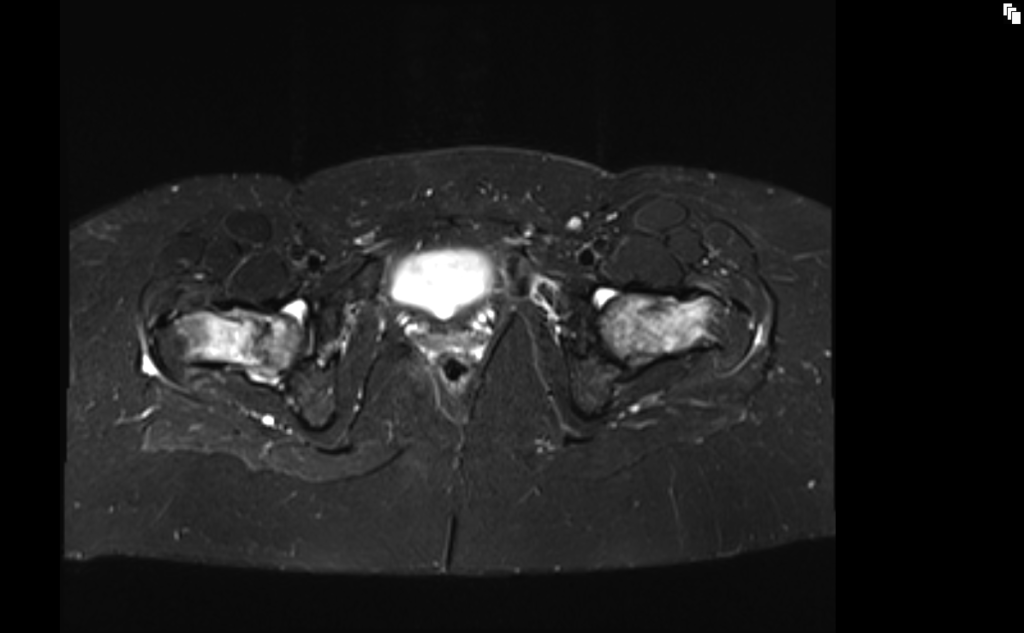
T1 axial image shows Bilateral hip fractures

References
- Pejic, A., Hansson, S., & Rogmark, C. (2017). Magnetic resonance imaging for verifying hip fracture diagnosis: why, when, and how? Injury, 48(3), 687-691. doi: 10.1016/j.injury.2017.01.025.
- Oka, M., & Monu, J. U. V. (February 2004). Prevalence and Patterns of Occult Hip Fractures and Mimics Revealed by MRI. American Journal of Roentgenology, 182(2).
- Efremov, K., Caterini, A., De Maio, F., & Farsetti, P. (2020). A simultaneous bilateral asymmetric hip fracture in an elderly patient: A case report and review of the literature. International Journal of Surgical Case Reports, 72, 377–380. doi: 10.1016/j.ijscr.2020.06.031. PMID: 32563825. PMCID: PMC7306533.
- Takagi, Y., Yamada, H., Ebara, H., Hayashi, H., Inatani, H., Toyooka, K., … Tsuchiya, H. (2022). Bilateral simultaneous asymmetric hip fracture without major trauma in an elderly patient: a case report. Journal of Medical Case Reports, 16(278). Published on July 16, 2022.
- Raval, P., Mayne, A. I. W., Yeap, P. M., Oliver, T. B., Jariwala, A., & Sripada, S. (2019). Outcomes of Magnetic Resonance Imaging Detected Occult Neck of Femur Fractures: Do They Represent a Less Severe Injury with Improved Outcomes? Hip Pelvis, 31(1), 18–22. doi: 10.5371/hp.2019.31.1.18
