MRI Cauda equina syndrome (CES)
Cauda equina syndrome (CES) is a serious neurological condition that occurs when the nerve roots in the cauda equina, a bundle of spinal nerves and spinal nerve rootlets at the lower end of the spinal cord, are compressed and disrupted. This can lead to severe lower back pain, neurological symptoms in the lower body, and even permanent impairment if not treated promptly.
Cause
CES can be caused by any condition that results in compression of the nerves at the end of the spinal cord within the spinal canal. Common causes include:
- Lumbar disc herniation: The most common cause, where a disc protrudes and compresses the nerve roots.
- Trauma: Accidents that cause fractures or dislocations of the spine.
- Tumors: Growth of masses inside the spinal canal can compress the cauda equina.
- Spinal stenosis: Narrowing of the spinal canal due to aging or degenerative diseases.
- Inflammatory conditions: Such as ankylosing spondylitis.
- Infections: Abscesses that develop in or near the spinal canal.
Symptoms
The symptoms of CES are often severe and acute, requiring immediate attention. They include:
- Severe lower back pain
- Sciatica: Radiating pain in one or both legs.
- Saddle anesthesia: Loss of sensation in the buttocks, perineum, and inner thighs.
- Bladder and bowel dysfunction: Inability to urinate or retain urine, and loss of bowel control.
- Sexual dysfunction
- Motor weakness and sensory loss in the lower extremities.
Diagnosis
Prompt diagnosis of CES is critical to prevent lasting damage. Diagnostic steps include:
- Medical history and physical examination: Checking for symptoms like saddle anesthesia and bladder dysfunction.
- MRI (Magnetic Resonance Imaging): The most effective imaging technique to visualize nerve compression in the spine.
- CT scan: Can be used if MRI is not available.
Treatment
Immediate treatment is crucial to prevent permanent damage:
- Surgical intervention: The primary treatment for CES is urgent decompression surgery to relieve pressure on the nerves. The type of surgery depends on the cause of the compression.
- Corticosteroids: May be administered to reduce inflammation in cases due to inflammatory processes.
MRI Appearance of Cauda equina syndrome
- T1-weighted MRI: On a T1-weighted MRI, normal bone marrow is usually high in signal intensity, appearing bright. In the case of spondylolisthesis, the slipped vertebra can be clearly identified. The alignment of the vertebrae is easily observable, and any associated changes in the bone marrow can be detected. For instance, if there is marrow edema or inflammation, it may appear as a lower signal area within the bright bone marrow.
- T2-weighted MRI: This sequence provides images where water content appears bright. It is especially useful for evaluating the condition of soft tissues, including discs, ligaments, and nerves. In the context of spondylolisthesis, T2-weighted images can help in assessing the degree of nerve root compression, if present, and the status of the intervertebral discs. It also aids in evaluating any associated conditions such as spinal stenosis or disc herniation.
- STIR (Short Tau Inversion Recovery): STIR is a special type of MRI sequence that is used to suppress the signals from fat. This makes it highly sensitive to changes in water content, thus highlighting areas of inflammation or edema (swelling). In spondylolisthesis, STIR can be particularly useful in identifying bone marrow edema, which might suggest an acute injury or stress reaction in the bone.
T2 sagittal image shows Cauda equina syndrome (CES)
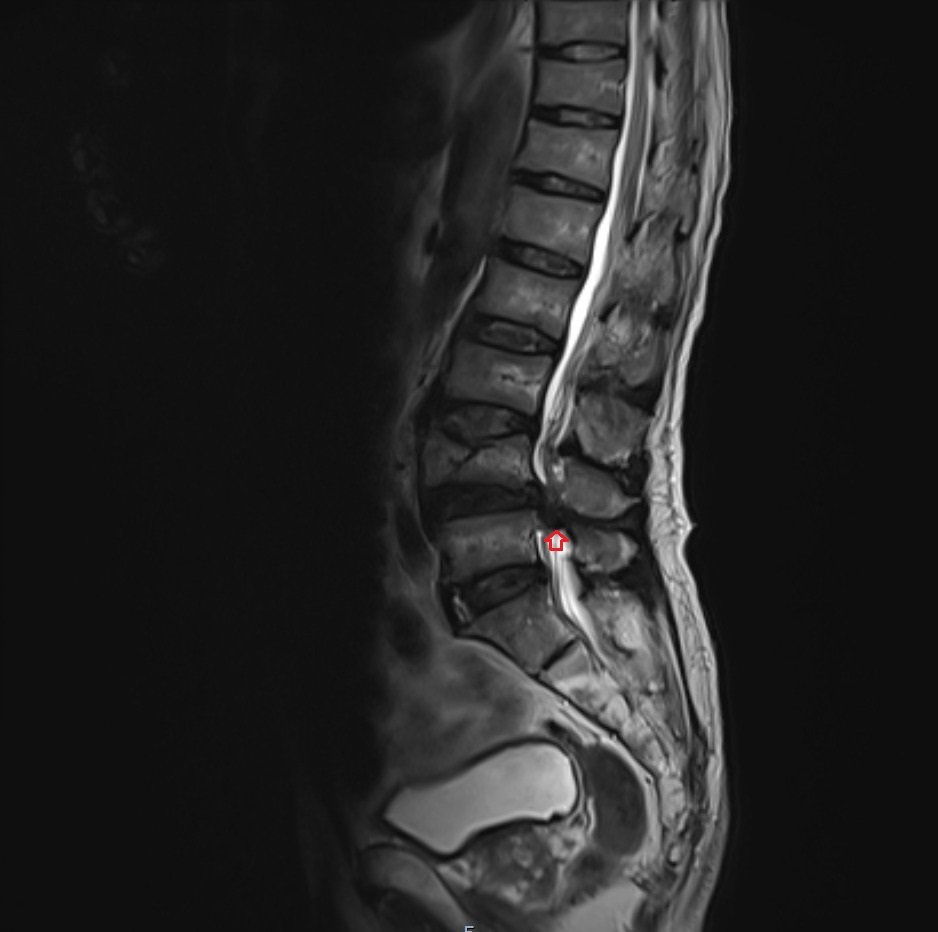
STIR sagittal image shows Cauda equina syndrome (CES)
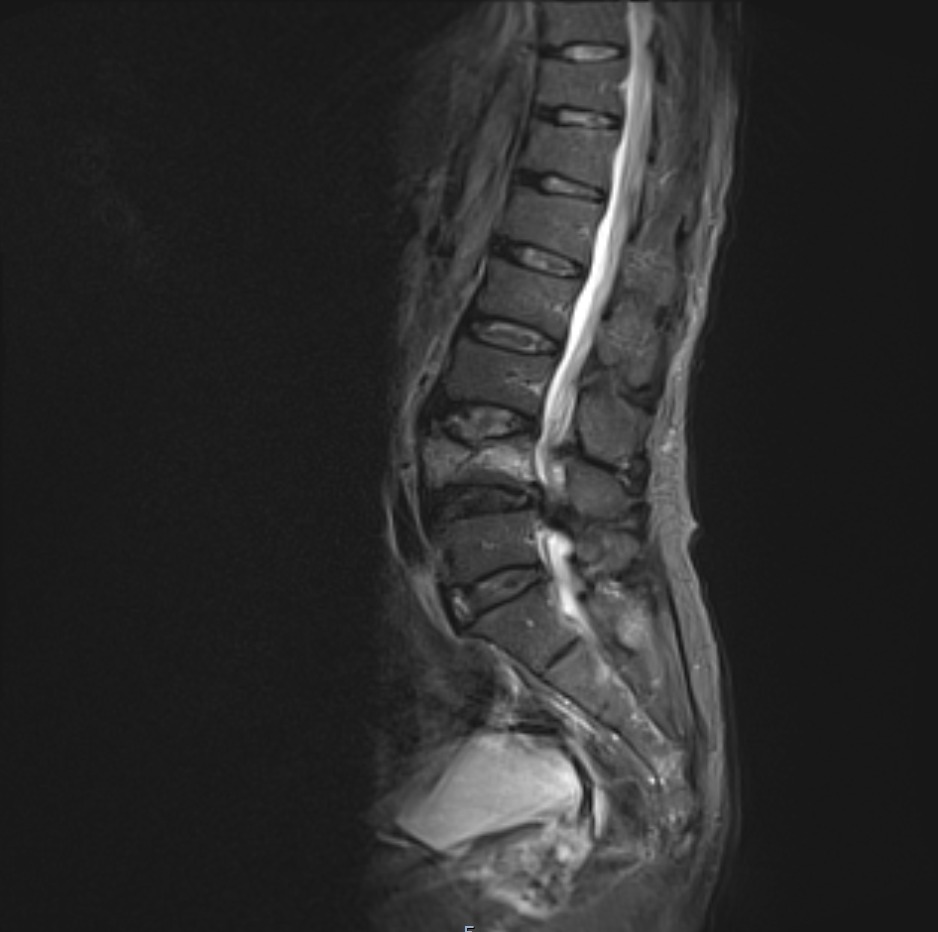
T1 TSE sagittal image shows Cauda equina syndrome (CES)

T2 TSE axial image shows Cauda equina syndrome (CES)

T1 TSE axial image shows Cauda equina syndrome (CES)
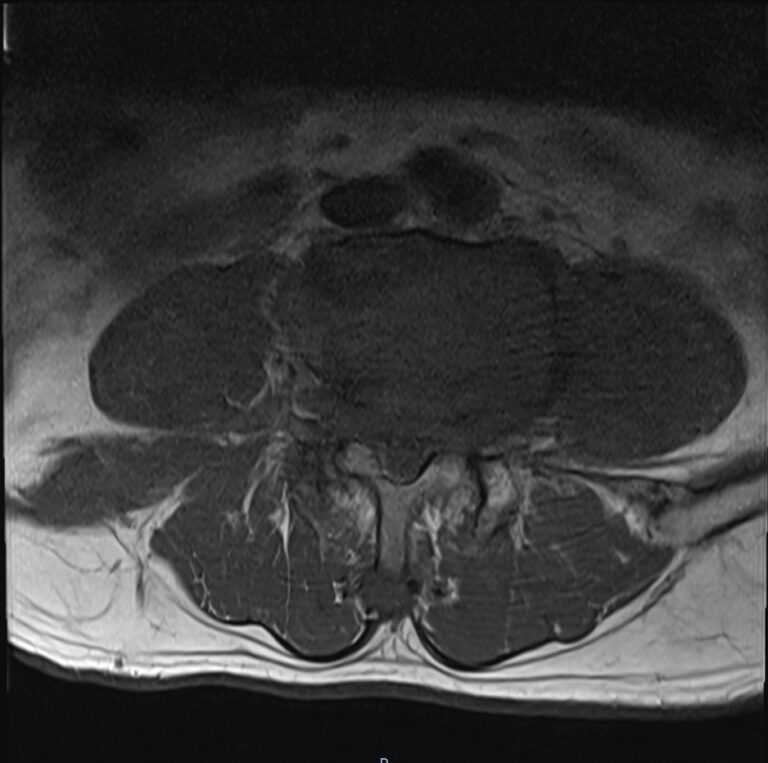
References
- McNamee, J., Flynn, P., O’Leary, S., Love, M., & Kelly, B. (2013). Imaging in Cauda Equina Syndrome – A Pictorial Review. Ulster Medical Journal, 82(2), 100–108. PMCID: PMC3756868. PMID: 24082289.
- Ahad, A., Elsayed, M., & Tohid, H. (2015). The accuracy of clinical symptoms in detecting cauda equina syndrome in patients undergoing acute MRI of the spine. Neuroradiol J, 28(4), 438–442. doi: 10.1177/1971400915598074
- Zusman, N. L., Radoslovich, S. S., & Yoo, J. U. (2020). Physical Examination Is Predictive of Cauda Equina Syndrome: MRI to Rule Out Diagnosis Is Unnecessary. Global Spine Journal, 12(2), 1-6. https://doi.org/10.1177/2192568220948804
